Spider Veins: What You Need to Know

What are spider veins?
Spider veins, also known as telangiectasias or thread veins, are small, dilated blood vessels that appear near the surface of the skin. They are called “spider veins” due to their web-like or branching pattern, which resembles the legs of a spider. These veins are typically red, blue, or purple in color and can be found on various parts of the body, but they are most commonly seen on the legs and face.
How are spider veins different from varicose veins?
Spider veins and varicose veins are both types of venous disorders, but they differ in several key ways, such as:
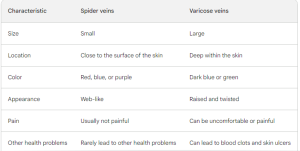
Who can get spider veins?
Anyone can get spider veins, but they are more common in women and people with a family history of the condition. Other risk factors include pregnancy, obesity, and standing for long periods of time.
What are the causes of spider veins
Spider veins develop primarily due to the weakening or damage of small blood vessels close to the skin’s surface. The exact causes of spider veins can be multifactorial, and several factors can contribute to their development. Some of the common causes and risk factors include:
- Genetics: A family history of spider veins is one of the most significant risk factors. Individuals with parents or grandparents who had spider veins are more likely to develop them.
- Age: As people age, the veins and their valves tend to lose elasticity and become less efficient at maintaining proper blood flow, increasing the risk of spider veins.
- Gender: Women are more likely to develop spider veins than men. Hormonal fluctuations during pregnancy, childbirth, menopause, and the use of oral contraceptives can contribute to this gender disparity.
- Hormonal Changes: Hormonal changes during pregnancy, puberty, and menopause can weaken the walls of blood vessels, making them more susceptible to dilation.
- Obesity: Excess weight puts added pressure on the veins, which can lead to the development of spider veins.
- Prolonged Standing or Sitting: Occupations or lifestyles that involve long periods of sitting or standing can hinder proper blood circulation and increase the risk of spider veins. Examples include nurses, teachers, and office workers.
What are the symptoms of Spider veins?
Spider veins are typically a cosmetic concern, and many individuals with spider veins may not experience any symptoms. However, in some cases, spider veins can cause mild to moderate discomfort and aesthetic concerns. Common symptoms and signs associated with spider veins may include:
- Visible Veins: The most obvious symptom is the appearance of small, dilated blood vessels on the skin’s surface. These veins often have a red, blue, or purple color and may resemble a spider’s web or tree branches.
- Itching: Some people with spider veins may experience mild to moderate itching in the affected area. This itching is often related to the pressure and dilation of the veins.
- Aching or Throbbing: Spider veins can cause a dull, aching, or throbbing sensation, especially after prolonged periods of sitting or standing. This discomfort typically lessens when the legs are elevated.
- Burning or Heaviness: Individuals with spider veins may sometimes report a sensation of burning or heaviness in the legs, particularly at the end of the day.
- Swelling: Swelling (edema) of the legs or ankles may occur in some cases, especially if the spider veins are associated with underlying venous insufficiency.
- Skin Changes: In more severe cases, spider veins can lead to skin changes, including dryness, discoloration, and the development of red or brown patches.
- Ulcers: Although rare, long-term neglect of spider veins can lead to the formation of skin ulcers, especially near the ankles. These ulcers can be painful and require medical attention.
How to diagnose spider veins?
A doctor can diagnose spider veins by performing a physical exam and asking about the person’s medical history. The doctor will look for small, dilated veins on the surface of the skin, usually on the legs or face. They may also ask the person about any symptoms they are experiencing, such as burning, tingling, or leg pain.
In some cases, the doctor may order additional tests to rule out other underlying medical conditions. These tests may include:
- Venous Doppler ultrasound: This test uses sound waves to create images of the blood vessels in the person’s legs. It can help to identify any problems with the blood flow in their veins.
- Plethysmography: This test measures the blood flow in the person’s legs. It can help to identify any blockages in their veins.
- Venogram: This test involves injecting a dye into the person’s veins and then taking X-rays. It can help to create a detailed image of their veins and identify any abnormalities.
Once the doctor has diagnosed spider veins, they will discuss treatment options with the person
How to treat spider veins?
The treatment of spider veins varies depending on the severity of the condition, the presence of symptoms, and individual preferences. Several treatment options are available, and the choice of treatment should be made in consultation with a healthcare professional or a dermatologist. Common treatments for spider veins include:
- Sclerotherapy: This is the most common and effective treatment for spider veins. A healthcare provider injects a special solution into the affected veins, causing them to collapse and gradually fade from view. Multiple sessions may be necessary for optimal results.
- Laser Therapy: Laser or intense pulsed light (IPL) treatments can target and seal off spider veins. Laser therapy is often used for smaller veins on the face. It can be less invasive than sclerotherapy and may require multiple sessions.
- Radiofrequency Closure: This method is used for larger varicose veins that have some associated spider veins. A catheter with radiofrequency or laser energy is inserted into the vein to close it.
- Pico Laser: Pico Laser treatment is a safe and effective solution for various pigmentary skin concerns. According to Dr Ng Hong Yi, aesthetic specialist in Singapore, this treatment can address various issues like spider veins, acne scars, sun spots, freckles, and the removal of unwanted tattoo ink. This modern laser treatment is renowned for its ability to rejuvenate the skin, resulting in a clearer, more radiant complexion.
- Compression Stockings: Wearing compression stockings can help alleviate discomfort and prevent the progression of spider veins. These stockings provide pressure to the legs, promoting better blood flow.
- Endovenous Laser Treatment (EVLT): For larger varicose veins with associated spider veins, EVLT involves the use of laser energy delivered through a thin fibre to close off the affected vein.
Spider veins are a common vascular condition that can affect people of various ages and backgrounds. While they are primarily a cosmetic concern, they can sometimes lead to discomfort and may be associated with underlying venous insufficiency. Understanding the risk factors, causes, symptoms, and available treatment options is essential for individuals seeking to address spider veins and maintain healthy, comfortable legs.
If you have concerns or symptoms related to spider veins, consult a healthcare professional or dermatologist for personalised guidance and to explore the most suitable treatment options to help you look and feel your best.




